So far we’ve discussed the complexities of pain, muscles and tendons…
now its time to do a bit of myth busting about joints.
What makes up a joint and why have you got pain?
Joints are structures/surfaces where bones meet. Typically when we have pain in our joints we experience it at the particular joints that have the most amount of freedom for movement, such as at the knees, hips or shoulders and the joints of the hands.
Joint pain can come from traumatic injury, overloading or overuse injuries, age-related changes or in some cases more systemic or whole-body issues. It is important to find out what the cause of joint-related pain comes from as this determines the best course of action for improving pain!
What is osteoarthritis
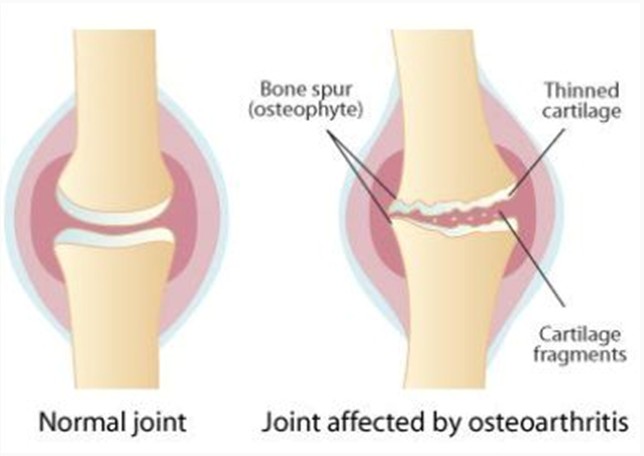
Osteoarthritis is a condition in which the protective cartilage surface of a joint changes in structure over time. Osteoarthritis has traditionally been described as a condition where the joint undergoes “wear and tear” and that we must reduce all activities that cause pain or we will make things worse – however this is not the case!
Many individuals with even severe osteoarthritis are actually asymptomatic and importantly, the level of cartilage breakdown (as seen on X-ray) does not correlate with levels of pain an individual may experience.
Simply put, osteoarthritis is not only a breakdown of cartilage structure but a whole-joint issue that must be addressed as such or problems can perpetuate!
When we have joint-related pain from osteoarthritis, pain can limit movement, which over time results in muscles becoming weak and deconditioned. This becomes a vicious cycle as everyday activities become increasingly harder to do.
Surprisingly enough, the joint-surface (cartilage) which changes in osteoarthritis actually needs loading to stay healthy; this structure does not have its own blood supply so needs a cycle of loading and unloading to give it the necessary nutrients to replenish itself. Some exercise is necessary to get the cartilage healthier and muscles stronger!
Do I need to rest?
Did running or activity cause it or make things worse?
Relative rest is ideal just like with tendons in our previous newsletter, doing something is better than avoiding all activity. It may be useful in the short term to reduce some provocative activities or modify how we are doing them but we have to start somewhere or getting back to meaningful and necessary physical activity will be near impossible!
Its unlikely that running or physical activity alone actually causes osteoarthritic joint changes; we now know there are plenty of other factors, some modifiable (lifestyle factors, being overweight, lack of physical activity, beliefs, fear) and others unmodifiable (genetics, age, sex) that are more plausible influences as to why individuals develop pain and symptoms related to osteoarthritis.
As discussed above, moderate loading/unloading cycles are needed for cartilage to stay healthy, muscles need exercise to stay strong and have capacity for activity, and bone also adapts and becomes more robust in response to load.
The idea that running and activity is “bad” for knees and hips is a myth!
Do I need an injection or surgery?
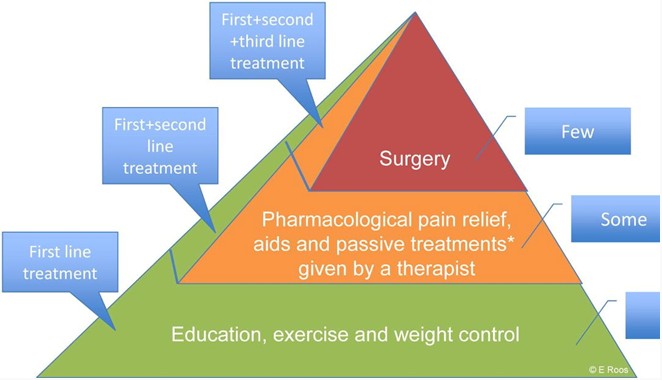
An injection such as cortisone may be useful in quelling pain in the short term however this is not a permanent solution and should be considered a 2nd-line measure that accompanies education, exercise and weight management!
As per the RACGP (Royal Australian College of General Practitioners) guidelines, all individuals with osteoarthritis should be offered these 3 treatment options first and foremost before trialling other 2nd-line or 3rd-line treatments as per the diagram above!
Injectables can be a useful tool for the right patient but only if pain is a significant barrier to participating in exercise. Much the same can be said for surgery, other options should be exhausted or trialled before this step is considered and there are associated costs and risks along with the supposed benefits… surgery is appropriate for the right patient and definitely does NOT come first.
So what do we do next? How do we exercise with painful joints?
How do I start exercising?
Its important that we optimally load muscles in such a way that the joint isn’t excessively aggravated; having guidance and help early on is crucial, especially since trialling new exercises can be a tricky process if you haven’t done any formal strength training in the past.
Land-based strengthening is key in order to restore strength and function to the joint adequate for the challenges of daily life which come with osteoarthritis. Exercise in the pool may feel good but does not prepare the body for the requirements of land-based activity.
The GLA:D program
The GLA:D program is a fantastic option for individuals suffering with hip and knee osteoarthritis; in the program physiotherapists guide patients through a set of simple land-based exercises which are relevant to tasks that osteoarthritis sufferers commonly have difficulty with. Over 2021 at Power Physiotherapy we ran several GLA:D exercise classes and education seminars with some pretty fantastic results!
Take Home Message! Whilst osteoarthritis is a lifelong condition, pain and disability doesn’t have to be! Exercise, education and weight management need to be the bread and butter of our rehabilitation before we consider more invasive treatments (which are costly, can be risky and don’t always work!).
Exercise and physical activity is safe to do even with some pain, as discussed in all of our previous newsletters in this series – pain does not equal more damage or harm is occurring to structures and to improve the situation, doing something is better than nothing at all!
The GLA:D program is a fantastic option for individuals with osteoarthritis of the hip or knee who are unsure about how to start exercising and enjoy a bit of a challenge!
If you would like to know more about osteoarthritis and how you can manage your joint-pain better, get in contact with us (reply to this email or give the clinic a call on 9440 6125) regarding our upcoming GLA:D education seminar!




